
via Google Maps

Audio By Carbonatix
Each year, about 5,000 Floridians are sent to one of the state’s seven mental health facilities. Some have been committed under the Baker Act for evaluation and treatment. Others are defendants found too mentally incompetent for a trial or guilty by reason of insanity. A smaller number are sexually violent predators deemed too dangerous to roam the streets.
By law, the state has a duty to treat those patients with dignity and respect. But a new audit reveals several serious shortcomings within Florida’s mental health institutions: The facilities are understaffed, unlicensed, and don’t meet building or fire codes.
The report also highlights lackadaisical protocols for securing millions of dollars’ worth of pharmaceuticals, in one case noting an inventory discrepancy of 2,840 antipsychotic drugs and 351 tablets of HIV antiretrovirals at the Florida State Hospital in Chattahoochee, just south of the Florida-Georgia line.
The Department of Children and Families is ultimately responsible for the seven facilities, three of which are directly managed by DCF and four of which are privately contracted. Last year, the state spent $303 million operating the hospitals.
The audit, which examined DCF from July 2014 to January 2016, confirms what Florida newspapers have been reporting for years. A Pulitzer Prize-winning story from the Tampa Bay Times and Sarasota Herald-Tribune reached many of the same findings in 2015, chronicling rising violence, sickening conditions, and dangerous staffing shortages within the hospitals.
But the recent report from the independent Florida Auditor General lays bare several new concerns. Despite a state law requiring hospitals and mental health institutions to be licensed by the Agency for Health Care Administration, auditors found that the state failed to obtain licensure for three of its facilities: the North Florida Evaluation and Treatment Center in Gainesville, the Treasure Coast Forensic Treatment Center in Indiantown, and two residential buildings at the Florida State Hospital.
Asked about the issue, DCF administrators told the audit team that the facilities weren’t licensed because the buildings didn’t meet building code or fire code and that bringing them up to code was too expensive.
Worse, the agency admitted it had stopped doing regular quality assurance reviews, leaving the task up to an accrediting agency that performed checks only every three years. Oversight of the facilities “was limited to reviewing specific incidents, such as mortalities,” auditors wrote.
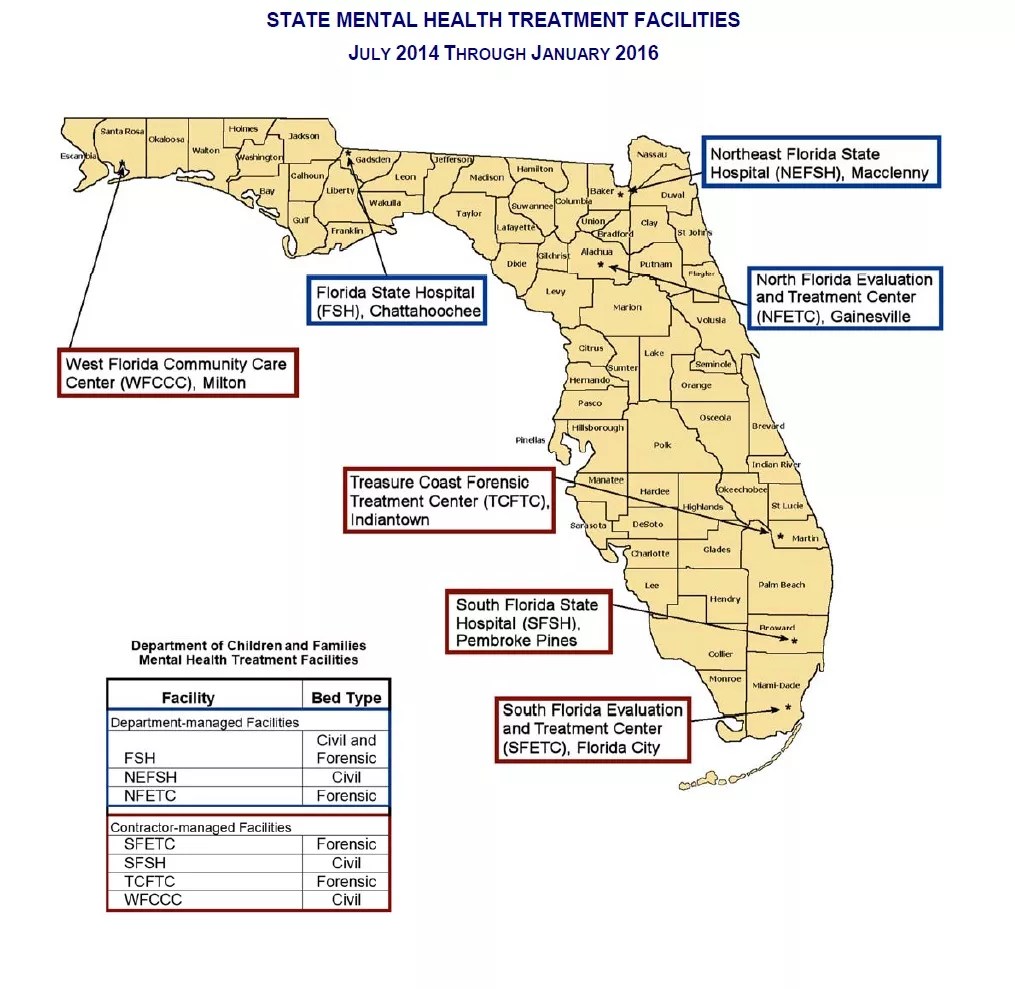
via State Audit
Other problems highlighted in the report:
Staff at the seven facilities failed to complete incident reports as required. In four cases, including two suicide attempts and two verified instances of abuse or neglect, employees waited more than 24 hours before contacting the state facilities director.- A review of 336 shifts at the Northeast Florida State Hospital showed that half were understaffed, by an average of three employees per shift.
- At two hospitals, the responsibility for ordering, receiving, and stocking pharmaceuticals fell to one person, leaving the opportunity for pills to go missing.
- The inventory system for tracking meds at Florida State Hospital was so out of whack that a physical count led to a discrepancy of 2,840 antipsychotic pills and 351 HIV antiretrovirals totaling $51,661.
- Ineffective procedures for dealing with and disposing of contraband like cell phones and drugs potentially allowed staff to take items home surreptitiously.
- Employees at Northeast Florida State Hospital used $11,229 to buy patients Christmas presents (which, though a nice gesture, isn’t an authorized use of funds).
- Separate pots of money for civil Baker Act clients and patients in the criminal justice system were used interchangeably, creating a misleading picture of the two operating budgets.
The deficiencies come as DCF has lost $100 million in funding, leading to a reduction of a third of its staff. In response to the audit, the agency has “sought legislative funding” to fix its facilities and is looking for ways to bootstrap some basic improvements within its current budget, says DCF Secretary Mike Carroll. Bringing the buildings up to code is estimated to cost anywhere from $45 million for the North Florida Evaluation and Treatment Center to $56 million to raze and rebuild Florida State Hospital, according to Carroll.
The department has promised to make changes and included in its response a timeline for doing so. Among the initiatives are bringing in a chief medical executive director, bringing back the regular quality reviews, starting a weekly call for leadership to talk about assaults, and moving to an online incident reporting system. Most of the improvements are expected to be completed by 2018.
At the state level, legislators have also shown some willingness to fix the situation. Last year, lawmakers allocated an extra $4 million for more staff at the facilities, though the loss of funding is likely to remain a problem this year as Gov. Rick Scott continues to slash the state’s budget.