Illustration by Pete Ryan

Audio By Carbonatix
The morning of June 20, Michael Morell woke up as he did every weekday, when his alarm clock rang at 6. The 34-year-old father of two sat up and reached over to his bedside table to hit snooze. But when he attempted to lie back down, his muscles became rigid, leaving him frozen in a sitting position. He was stuck.
The convulsions began in his upper body and moved up through the muscles in his cheeks, which started to twitch uncontrollably. In a matter of moments, Morell’s body began to shake so hard it woke his wife. As he smacked his lips over and over again, Tania Gonzalez asked her husband if he was OK, but he didn’t reply. He just stared straight ahead, eyes open, unresponsive.
“It’s weird because I didn’t feel like there was anything wrong in that moment, but I was confused as to why I was in an upright position,” Morell recalls. “The next thing I remember is being in the hospital bed with my family surrounding me.”
Morell, who had previously been diagnosed with epilepsy, was experiencing a tonic-clonic seizure, also known as grand mal. Unable to snap her husband out of his trance, Gonzalez frantically called an ambulance. EMTs rushed to the couple’s home in Homestead and transported Morell to the nearest emergency room, at Homestead Hospital.
Upon his arrival, doctors with Baptist Health, which runs the hospital, gave Morell morphine, prompting an additional seizure. His attending physician ordered a series of medical tests, including a CT scan, MRI, EKG, and toxicology test. The CT and EKG tests were unremarkable, but the MRI showed a four-millimeter cyst in the mesial temporal lobe of Morell’s brain.
Doctors received the MRI results at 4:49 that afternoon. Three hours later, psychiatrist Daniel F. Mandri stopped by Morell’s hospital bed for a visit. But it wasn’t the MRI results that Mandri wanted to talk about.
“At first, I didn’t think anything was off, but then he started asking me weird questions,” Morell remembers. Mandri asked if he did any illicit drugs. Morell said no. But then the psychiatrist got more specific, asking if he “did cannabis.” Morell was honest: He told Mandri, yes, he used medical marijuana prescribed by a doctor to treat his epilepsy and occasionally smoked joints to calm himself.
“Yes, I smoke weed,” Morell says. “But I have a license and a full green light to do this legally.”
That fact apparently didn’t sit well with the hospital. Mandri was “asked to see patient for ‘drug abuse and seizures,'” according to consultation notes Morell provided to New Times. The next day, the attending physician, Dr. Jimena Amparo Blandon, also paid Morell a visit. By Blandon’s estimation, Morell had a serious problem – cannabis abuse disorder.
“Yes, I smoke weed,” Morell says today. “But I have a medical marijuana license and a full green light to do this legally.”
November marks three years since Floridians passed Amendment 2 with a popular vote of 71 percent, establishing a medical marijuana program in the Sunshine State. To date, more than 327,000 patients have qualified for medical cards, including Morell. Now that medicinal marijuana is a reality for sick residents across the state, activists are busy waging the next battle in the war: circulating a petition to put recreational pot on the ballot in 2020.
Bias and misinformation, however, have a devious way of lingering long after laws have changed. Although epilepsy is listed as one of the “debilitating medical conditions” in the state’s constitution – making it legal to treat with medical marijuana – some Florida institutions are still treating prescribed cannabis as an illicit drug.
Homestead Hospital declined to comment on Morell’s case, citing patient-doctor privilege, and multiple attempts to contact Mandri and Blandon went unanswered. But Karen O’Keefe, director of state policies at the Marijuana Policy Project, says hospitals are caught in a “federal Catch-22.” The U.S. government defines cannabis as a drug with no accepted medical use, and hospitals could face penalties and lose federal funding for allowing patients to use medical marijuana. As long as marijuana remains a Schedule I controlled substance, hospitals are stuck.
“It’s a problem,” O’Keefe says.
Shortly after his conversation with Blandon, Morell asked to be discharged from Homestead Hospital. His exit paperwork included a four-page guide to cannabis abuse disorder and a recommendation that he go to a treatment facility. His bill for the 24-hour stay? More than $60,000 before insurance.
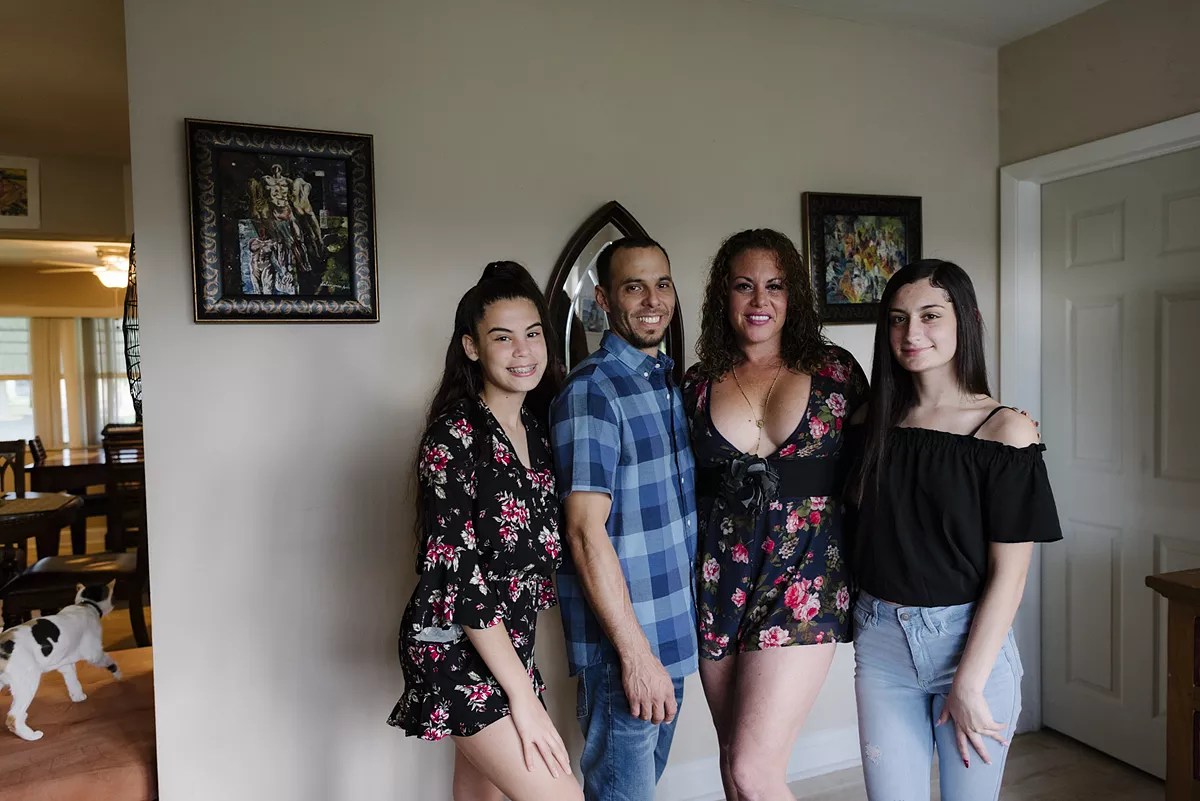
Michael Morell with his fiancée Tania Gonzales and her two daughters.
Photo by Karli Evans
Morell and Gonzalez were on a church philanthropy trip in Orlando when he had his first epileptic episode in November 2018. They were lying in bed when Morell’s body began to jerk involuntarily. Quick to act, Gonzalez flipped him onto his side and placed the corner of a pillow in his mouth so he wouldn’t bite his tongue.
Morell woke up the next morning in a bed at Florida Celebration Hospital. It took him a while to remember what happened, he says. Ultimately, he was diagnosed with epilepsy, a seizure disorder that runs in his family.
The diagnosis weighed heavily on Morell in those early days. He was terrified about the future, thinking back to his childhood in Kendall when his father died of melanoma. Above all, he worried about his wife and daughters.
“I don’t want them to go through the same thing I went through,” he says. “I can imagine it’s very scary for them to see me go through all of this.”
Long before they fell in love, Morell and Gonzalez knew each other as kids. Morell’s aunt used to babysit Gonzalez, whose father lives a block away from the Morell family. Gonzalez, now 38, went to elementary school with Morell’s older brother Erick and became close friends with her future husband during high school.
After graduation, Gonzalez and the Morell brothers fell out of contact. Michael Morell, who remained in South Florida, began working at a marine repair facility. Gonzalez, meanwhile, joined the military and moved to Pennsylvania, where she eventually married and had two girls. After that marriage ended in divorce, Gonzalez moved back home at the end of 2013.
As long as marijuana remains a Schedule I controlled substance, hospitals are stuck.
The old friends finally saw each other again at a 2014 New Year’s Eve party – the date now designated as the beginning of Gonzalez and Morell’s romantic relationship. Erick Morell says he watched from across the room as his brother and Gonzalez “just clicked.”
“She’s the best choice my brother has ever made,” Erick Morell says. “She’s become the cog in this big, crazy family we have.”
At first, Gonzalez was apprehensive about the courtship. Her divorce had been hard, and she didn’t want to suffer heartbreak again, nor did she want to lose a friend. She was also in “mommy mode,” she says, and worried about introducing a new man into her children’s lives. But spending time with Morell brought her comfort and joy. He was respectful and trustful, and he knew her well. She says it just felt right as the two naturally progressed from friends to lovers and ultimately to family.
“It was destined,” Gonzalez says. “I ended up finding love where I didn’t expect it, and I’ve never looked back.”
Her beloved “Mikey” was quickly accepted by her teenage daughters. He helps handcraft T-shirts for their cheerleading team, takes them camping, and goes to every school event and PTA meeting. “We’re not just a family – we’re a team,” Gonzalez says.
After Morell’s epilepsy diagnosis, the family modified its lifestyle to fit his medical needs. Gonzalez credits her upbringing as an “Army brat” for her quick response whenever Morell has an epileptic episode. Morell’s mother chips in with driving and cooking when she can, and Morell points out that his daughters no longer groan when he asks them to clean their room or do their laundry.
For Morell, the most difficult part of having epilepsy is his inability to drive. In Florida, drivers must be seizure-free for six months before they can get back behind the wheel. The requirement necessitated that Gonzalez shoulder the burden of taking the girls to and from school and shuttling them to cheerleading practice and weekend classes at Miami Dade College.
“It’s tough because Tania has to do all the driving,” Morell says. “It’s not a great feeling to know you can’t pick up the slack.”
Early on his treatment, Morell was prescribed Keppra, a widely used seizure medication that attaches itself to a protein in the brain to better regulate the release of chemicals. But it doesn’t work for everyone, and Morell began to experience significant side effects. Keppra was not the answer to his woes, and within a month, he was back in the emergency room with another epileptic episode.
This time, Morell decided to change tactics. Believing Keppra was too aggressive for him, he spoke with his neurologist and decided to try medical marijuana. To receive his card, Morell had to show proof of his epilepsy diagnosis via medical records, obtain a doctor’s recommendation, and present a valid Florida driver’s license.
The marijuana nasal spray he was eventually prescribed contains only 5 mg of the cannabinoid tetrahydrocannabinol (THC). Yet one spray is all he needs to prevent his symptoms from accelerating and extend the time between seizures.
Almost immediately, Morell felt better. By late May, he was able to drive himself to work again.

Morell in his Homestead home.
Illustration by Pete Ryan
Since his diagnosis, Morell has learned to recognize the warning signs of an impending seizure. First, there’s a sudden onset of an indescribably weird smell, he says. Visual disturbances follow next, and flashes of light flicker like an aura before a migraine. Darkness appears along the outer edges of his eyesight, a black that quickly closes in toward the center until he can barely see. Then comes the epileptic episode.
Although epileptic seizures are more common in childhood, it’s not unheard of for the disorder’s onset to begin in adulthood.
“People get epilepsy at any age,” explains Jacqueline French, chief science officer at the Epilepsy Foundation and a professor of neurology at New York University’s Langone Medical Center. “Someone with adult onset epilepsy can be healthy their entire life until they have a seizure.”
The brain is an incredibly complex organ, and French describes it as “like an electrical current.” Seizures occur when brain cells are abnormally communicating with one another. But modern medicine still does not know definitively how and why epilepsy forms.
Nevertheless, during his stay at Homestead Hospital, Morell was warned that marijuana “lowers the threshold” for epilepsy, he says.
“During the evaluation the patient is explained that Marijuana may worsen presentation of seizures, he is upset about this recommendation because he has been prescribed marijuana by his neurologist [sic],” Blandon, the attending physician, wrote in the discharge summary papers for Morell, which he provided to New Times.
“A doctor is responsible for the health of a patient… If they’re making a moral decision, that’s wrong.”
French acknowledges some epilepsy patients use THC and cannabidiol (CBD) to treat their medical conditions. “Scientists are not all in agreement that marijuana helps with seizures,” she says. “But we also do not know definitively that it doesn’t help either.” The FDA approved Epidolex, an oral CBD solution for the treatment of seizures, in June 2018.
Over the course of his hospital stay, Morell’s medical records show doctors repeatedly tried to give him opioid-based narcotics. After Morell complained of a headache, doctors wanted to give him Percocet every six hours, recommending an oral tablet ranging from 5 mg to 325 mg. They also recommended he take 5 mg of the sedative zolpidem (also known as Ambien) at bedtime even though he does not suffer from insomnia. Morell says he refused the Percocet and zolpidem and asked for Tylenol instead.
Morell says he was also warned that marijuana could cause schizophrenia, a theory that has not been scientifically proven. A 2014 Harvard Medical School study showed that a genetic predisposition to psychosis – not cannabis – was the fundamental cause of schizophrenia in patients who had used cannabis.
“Society as a whole has increased its use of marijuana, but the rate of schizophrenia has not changed,” O’Keefe says. “It’s likely more correlation than causation, but, unfortunately, there’s still a lack of education and bias against ‘reefer madness.'”
“Doctors and hospitals need to understand that marijuana is a medicine,” adds Karen Goldstein, the executive director of Florida’s chapter of the National Organization to Reform Marijuana Laws (NORML). “They need to update their policies.”
Although Goldstein has not heard of a similar case in which a medical marijuana patient with epilepsy was labeled a drug abuser, she’s not surprised it happened. “Lots of people are getting relief from seizures with marijuana,” she says. “A doctor is responsible for the health of a patient regardless of the cause. If they’re making a moral decision, then that’s wrong.”
For his part, Morell refuses to give up hope after his negative experience at Homestead Hospital. Following his release, he scheduled an appointment to see a new doctor at a different medical facility to evaluate the cyst in his brain.
“I was feeling really helpless before,” he says. “I felt like a Ping-Pong ball getting tossed from one side of the table to another. But I’m feeling more hopeful now.”
These days, Morell usually takes the bus to work or uses Lyft. He’s now managing the marine repair facility where he’s worked since 2000. It’s a family-run business, and he’s grateful his employer had been understanding about his medical struggles. He’s taken time off with no questions asked, and his employer even helps pay for half of the Lyft rides he takes into work.
Through it all, Morell credits his family’s emotional support with keeping him steady. “It’s really a beautiful thing,” he says. “It’s not just my own household, but my mom, brother, stepbrothers, and sisters have all come out of the woodwork to call me and check in on me. It’s brought a lot of us closer together.”