

Audio By Carbonatix
In March of 2020, Jackie, a tour guide from Miami, had just finished leading a three-month trip across Africa for a small group of travelers. Exhausted from the whirlwind adventure, she planned to take it easy in Cape Town for a while – enjoy the local dining scene and visit a few wineries. Sure, she’d heard of the coronavirus, but as far as she was concerned, that was a problem happening on an entirely different continent.
“I just kind of assumed it was contained to China and it wouldn’t go much farther than that,” she says.
But the virus had other plans. The World Health Organization soon declared COVID-19 a pandemic. Governments the world over implemented drastic interventions. Two days after Jackie crossed into South Africa from Namibia, the country closed its borders and started grounding flights. By some stroke of luck, she managed to get a seat on one of the last planes back to Florida.
At that time, Miami was just beginning to buzz with panic. As Jackie quarantined in an Airbnb, the landscape around her started shifting. On March 17, Miami-Dade shut down restaurants. Two days later, it was public parks and beaches. Then it was nonessential businesses. On March 26, then-County Mayor Carlos A. Giménez issued an order urging residents to stay at home “other than to engage in essential activities.”
We all know what happened next.
As we confront the one-year anniversary of COVID in Miami, New Times is looking back on the past 12 months of pandemic life. We spoke with folks who experienced fear, loss, sickness, exasperation, anger, and loneliness. But, like many of us, they also harbor hope. With the arrival and deployment of three efficacious vaccines, there’s an optimism that this year will be better than the last.

In the early days of the pandemic, testing supplies were scarce.
Photo by Joshua Ceballos
Eric Johnson, who leads the union that represents Hialeah firefighters, says the early days of the pandemic were like going into battle armed with nothing more than a stick and a shield. There weren’t enough masks to go around, and other personal protective equipment was scarce. About 60 firefighters out of the department’s 220 contracted the virus on the job. A few months ago, one firefighter came down with it, and three of his family members got sick and died.
The fear of COVID never ceased. But as supplies and testing became more readily available and first responders acclimated, they felt better prepared to fight the war.
“Now we have machine guns and hand grenades and body armor,” Johnson says. “PPE is our body armor. We have enough. We’re much safer and better protected than in the beginning. We can walk into a house with 13 people who have COVID. When we’re done, we decontaminate the trucks, take a shower, change, and answer the next call. We went to a house just last week with four or five people with COVID. You go in there, do your damn job, and get the fuck out.”
“You go in there, do your damn job, and get the fuck out.”
Monica, who works at a Miami healthcare center, says part of being a first responder is pushing past fear to do your job, even when that fear is warranted.
Whereas normally she would jump at a moment’s notice to help a patient, during the first few months of the pandemic, apprehension about the new virus had her questioning her every move.
“I had a patient stop breathing, and there was some hesitation now with COVID. Do you want to give this patient CPR, or do you want to be in fear? You’re doing chest compressions and there’s nothing over the patient’s mouth, but you have to save them so you jump into action.”
Even now, Monica’s days are spent pulling 12-hour shifts, wearing facemasks at all times, and frequently having to don a hazmat suit. After so long on her feet wearing protective equipment, she often gets headaches and feels lightheaded.
Although she knows it’s important to take breaks for her own health, sometimes those breaks don’t come. She’s still busy enough that she and her coworkers often forget to take lunch.

While virtual schooling is in many ways more accessible, it lacks the intimacy of a classroom.
Photo by homegets.com/Flickr
Behind the front lines, workers in other fields have faced their own challenges.
One woman who lost her job in the travel industry has struggled to buy groceries and pay the mortgage while begging for relief from the state’s notoriously broken unemployment system.
“I stopped receiving unemployment insurance benefits in December because Florida’s unemployment system, due to technical issues, cannot update my claim,” she told New Times in an email. “Every time I call customer service [at the Florida Department of Economic Opportunity], I am being told the back office is very busy and they are allowed to escalate only once per month…. It has been more than two months that they are working to update the system and have not paid any benefits, state or federal.”
Others spoke of the lonely isolation of remote working and learning. One graduate student told New Times that while virtual schooling is in many ways more accessible, it lacks the intimacy of a classroom.
“For me personally, it has been a challenge, for I greatly enjoy face-to-face learning and being able to make new connections and build bridges with classmates and colleagues that come from all different kinds of backgrounds and walks of life,” he wrote in an email. “It’s just not the same to ‘meet’ someone through Zoom or camera.”
“It’s just not the same to ‘meet’ someone through Zoom or camera.”
That isolation has been especially exacerbated for people who previously had little contact with the outside world. Detainees in Immigration and Customs Enforcement (ICE) facilities had already been one step removed from their family and friends, but when the pandemic hit, they lost in-person visitation, as well.
Advocacy groups used to be able to regularly visit facilities like the Krome Detention Center in southwest Miami-Dade. Volunteers would buy books for the detainees and deposit money into their accounts so they could make calls. The point was for them to not feel so lonely, like someone was looking out for them.
Thomas Kennedy, a formerly undocumented immigrant turned activist, says immigrant detention has always been a cruel and inhumane place, and COVID-19 has only made things worse. Some advocates and volunteers aren’t sure how to make a difference from a distance.
“I recently had someone reach out to me saying that they want to do visitation,” Kennedy says. “I had to tell them we can’t do that.”
Bud Conlin, program coordinator for the Immigrant Action Alliance, says the detainees at Krome feel even more cut off than usual.
“They do tell us they miss us and would love a visit,” Conlin says. “We’re focusing on what we can do – staying in regular contact.”

Caring for patients with COVID-19 has its own challenges.
Even without the limitations of lockup, many Miamians have been physically separated from their loved ones. Ana, who works as a nurse, regularly tends to patients – many of them elderly – whose families aren’t allowed to visit. In a way, her own situation is not so different.
“My brother was in Brazil when he got COVID,” she says. “He was hospitalized on a Friday, and he died a week later. Then my dad got COVID around the same time in Texas, and he was in the ICU for a week and a half. Then my sister who was caring for him got it.”
Before, Ana’s family had only been a flight away. But amid an unprecedented health crisis, traveling to visit them wasn’t an option.
“I couldn’t take time off because of the pandemic. This was one of the greatest struggles between my profession and my personal life,” she says. “We haven’t been able to give my brother a proper burial.”
One of the hardest things, she finds, is seeing people downplay the virus that has taken so much from her family and upended her life.
“It makes me sad when people don’t wear masks or comply with rules, because they don’t understand the cost, and I get infuriated when I hear people talking about not getting the vaccine,” she says. “If they only knew what it is like to really lose somebody to something we can at least try to prevent, maybe they would be more aware.”
After contracting COVID this past November, Jackie, the tour guide who managed to get out of Africa, feels similarly. After coming back to Miami in March, she returned to work for her previous employer, a lawyer. Because it was a small office with just a handful of employees working at a distance from one another, she felt relatively comfortable with the setup. But although she and her coworkers wore masks and got tested weekly, she still managed to contract COVID at the office.
Months later, Jackie is still physically recovering, which is why it’s been frustrating to watch others carry on as if everything is normal.
“It’s a little bit difficult to see everybody behaving como si nada – like nothing’s going on outside,” she says. “You don’t want to get this, and you don’t want to give it to people. And people don’t seem to care.”
“You don’t want to get this, and you don’t want to give it to people. And people don’t seem to care.”
After she tested positive, Jackie isolated in her bedroom so she didn’t pass the virus to her father, with whom she lives. She was congested and had a raging headache, but the most pervasive and frightening symptom was a sudden inability to breathe. During those first few weeks, Jackie, a smoker, obsessively checked her oxygenation levels with a pulse oximeter.
“I was gasping for breath,” she says. “You hear all these horror stories about what COVID can do to you. People were dying. It’s a little bit terrifying. I was just trying to focus on getting through it.”
After two weeks in quarantine, eating meals her father left outside her door and passing the time watching The Repair Shop, a British show about bringing antiques back to life, Jackie tested negative. But she never really got better. She went through a phase where she was sleeping up to 16 hours a day. She visited urgent care and the emergency room seeking treatment on a few occasions when she felt like she couldn’t breathe. She took high doses of an anti-inflammatory medication that caused her to develop cataracts.
“Three weeks ago, I had cataract surgery. I feel like shit again,” she says. “I can barely ride my bike. I think this is just gonna be months and months more, if not forever, of me dealing with this.”
Since coming down with COVID, Jackie has tried to take more control over her health. She’s gone vegan, and she doesn’t smoke anymore. She recently got vaccinated, but she’s not sure when – or if – her life will return to the way it was before 2020.
“I miss my life,” she says. “I would love to sit in a café with a coffee and a cigarette – that’s the dream. But I don’t really want a cigarette; I just want to be able to breathe again.”
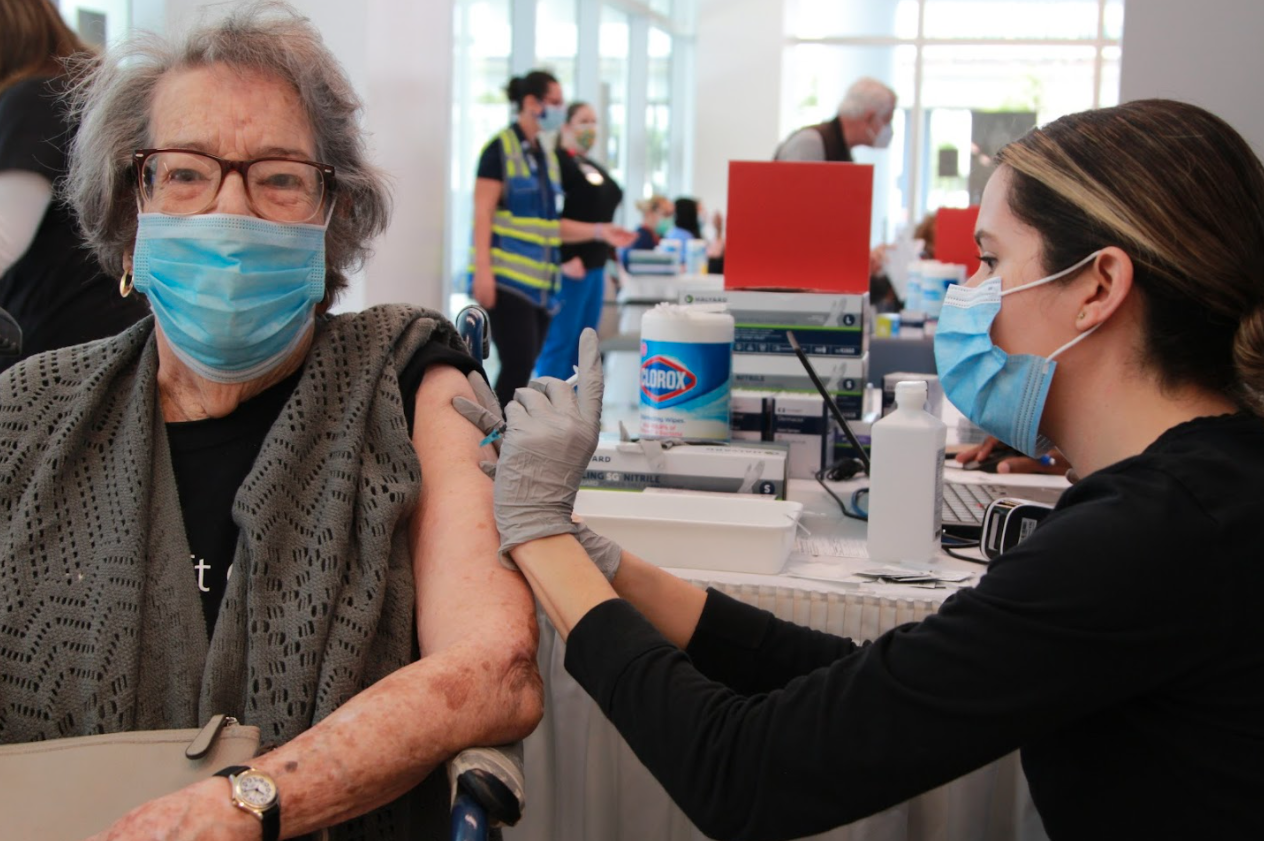
More people are becoming eligible to receive the COVID-19 vaccine in Miami-Dade.
Photo by Jeremie McLeod/Jackson Health System
To date, more than 4.3 million Floridians have received at least one dose of COVID vaccine, including more than 539,000 in Miami-Dade County. Eligibility restrictions seem to be loosening every week, and production is ramping up. Each shot administered is a portal out of the “new normal” and back to just… normal.
Each shot administered is a portal out of the “new normal” and back to just… normal.
Kathleen Sposato, director of infection prevention at Jackson Health System, received her second dose of the COVID vaccine at the beginning of January and counted down the 14 days until she was considered fully immunized.
Then she traveled to New York to see her three children and her grandson for the first time in more than a year.
“It was amazing,” she says. “I saw [my grandson] when he was 9 months. That was my last visit. He’s almost 2 now.”
Seeing her family in person after a whole year felt significant. Sposato says the past year has been a lonely one for her, just as it has been for many others. It was also a year filled with hard lessons.
One of the greatest takeaways for her has been that pandemics can’t be treated solely as a medical problem – any future outbreak must be addressed as a social and economic problem, too. She says governments need to build stronger safety nets for people who may lose their jobs or fall ill for long periods.
“We’ve learned that we are a community and no man is an island,” she says. “What I do affects everyone around me, and what the people around me do ultimately affects me. Not just with public-health measures but with helping people. I would hope next time we have a pandemic, we’re more proactive with early support for vulnerable individuals. We’re responsible for our neighbors, and it’s not just by wearing masks. It’s with making sure they have food to eat and a place to stay.”
Sposato finds it encouraging that this year, there has been virtually no spread of the flu because people are masking up in public, keeping their distance, and washing their hands.
“I’m pretty impressed with the way this community has really been responsible about using PPE,” she says. “Despite being optimistic, I am a little concerned about relaxing standards too soon. We are immunizing at a pretty fast rate. The more people who are immunized, the closer we are to relaxing those standards. I know there is an exhaustion when it comes to all the behaviors we have asked people to engage in to be safe. We’re not at that point yet, but we will be soon – if we can hang on a little bit longer.”